Cerebral microangiopathy: symptoms, causes and treatment
For our brain to stay alive and function properly, it needs a constant supply of oxygen and nutrients (especially glucose), which we obtain through respiration and feeding. Both elements reach the brain through the irrigation carried out by the vascular system.
However, injuries and damage sometimes occur that cause blood vessels to stop working properly or break down. One of the disorders that causes this is brain microangiopathy .
- Related article: "The 10 most frequent neurological disorders"
Cerebral microangiopathy: Concept and typical symptoms
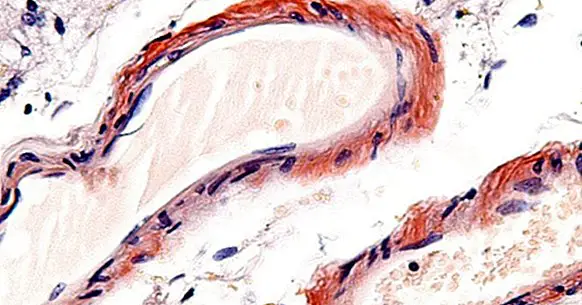
Brain microangiopathy is understood to be any disorder characterized by the presence of lesions or alterations in the part of the vascular system that supplies the brain. Specifically, reference is made to small blood vessels, arterioles and venules, which are ultimately the closest to and in contact with the target areas.
In this type of disorders the walls of these blood vessels may become brittle and break , easily producing brain hemorrhages that can cause a variety of symptoms depending on the area where they occur.
The most typical symptomatology of these disorders, which derives from the moment in which cerebrovascular accidents occur, includes paralysis of part of the body, alteration of speech, the presence of continuous headaches, dizziness and vomiting, loss of consciousness and slowing down of speech and of the movement. Epileptic seizures and seizures, sensory losses, altered moods, and even hallucinations and delusions may occur.
Cerebral microangiopathy It is not deadly in itself, but the cerebral infarctions it facilitates are very dangerous and can lead to the arrival of cardiovascular dementias, incapacitation and even the death of the patient. Symptoms usually do not occur before the age of forty-five, mostly leading to more advanced brain accidents. However, there are cases in which they have occurred even in childhood.
Types of cerebral microangiopathy
The term cerebral microangiopathy does not designate a disease in itself, but rather refers to the set of disorders that cause an altered state of the small blood vessels .
Thus, within the microangiopathies of the brain can be found various syndromes and disorders, three of which we present below.
1. Autosomal dominant cerebral arteriopathy with subcortical infarcts and leukoencephalopathy (CADASIL).
Better known by its acronym, CADASIL, this disease of genetic origin affects especially the arterioles that are connected to the subcortical nuclei of the brain, especially in the basal ganglia and around the ventricles .
The muscles of the walls of these blood vessels degenerate progressively, losing elasticity and breaking easily. It is a hereditary disorder of an autosomal dominant nature, caused by mutations in the NOTCH3 gene.
- Related article: "Basal ganglia: anatomy and functions"
2. Cerebrotaretinal microangiopathy with cysts and calcifications
Infrequent disease that causes various types of alterations in the connections between the visual organs and the brain , in addition to facilitating bleeding problems in the digestive tract. The main characteristics of this disorder is the presence of cysts and calcifications in the thalami, basal nuclei and other subcortical regions in both hemispheres. The first symptoms usually occur during childhood, evolving rapidly. Its origin is found in mutations of the CTC1 gene of chromosome 17.
3. Susac syndrome
Another disorder caused by microangiopathy is Susac syndrome. It is generated by a non-inflammatory microangiopathy whose main effects are at the cerebral, retinal and auditory levels, affecting the blood vessels that connect between these areas. It usually causes hearing and visual losses. It is suspected that its origin can be found in autoimmune causes , although its exact etiology is still unknown.
Causes
The specific causes of each microangiopathy will depend on the type of disease or disorder that occurs.
In many cases, as with CADASIL, the causes of this disorder are of genetic origin, presenting mutations in genes such as NOTCH3 or COL4A1 . However, they can also be produced and / or favored by acquired factors.In fact, diabetes, obesity, high cholesterol and high blood pressure have an important role both in developing it and in aggravating the prognosis of cerebral microangiopathy, assuming relevant risk factors and taking into account when explaining some of these disorders and in some cases being its direct cause. Certain infections can also alter and damage blood vessels.
It has also been documented the presence of a high amount of lipoprotein A in many cases of vascular accident, contributing an exaggerated amount of this substance to the facilitation of thrombi.
Treatment
As with the causes and even the symptoms, the specific treatment to be applied will depend on which zones are damaged. In general, microangiopathies do not usually have a treatment that reverses the problem. But nevertheless, prevention is essential both in the case of having a disorder or problem that facilitates the weakening of the blood vessels (especially it is necessary to monitor in those cases that suffer hypertension, obesity and / or diabetes). That is why it is recommended to establish healthy lifestyle habits.
Apart from that, different therapeutic strategies can be applied to alleviate the symptoms and maintain stronger blood vessels. It has been shown that the application of corticosteroids in a continuous way can improve the condition of patients . Also other substances allow to improve the symptomatology, as. Rehabilitation after an ischemic accident and psychoeducation to the affected and their environment are other fundamental factors to consider.
Bibliographic references:
- Aicardi J. (3rd Ed) (2009). Diseases of the Nervous System in Childhood. London: Mac Keith Press.
- Kohlschüter A, Bley A, Brockmann K, et al. (2010). Leukodystrophies and other genetic metabolic leukoencephalopathies in children and adults. Brain Dev. 32: 82-9.
- Herrera, D.A .; Vargas, S.A. and Montoya, C. (2014). Finding by neuroimaging of retinal cerebral microangiopathy with calcifications and cysts. Biomedical Magazine. Vol.34, 2. National Institute of Health. Colombia.
- Magariños, M. M .; Corredera, E .; Orizaola, P, Maciñeiras, J.L. (2004) Susac syndrome. Differential diagnosis Med.Clin .; 123: 558-9.
- Madrid, C .; Arias, M .; García, J.C .; Cortés, J. J .; López, C. I .; Gonzalez-Spinola, J .; From San Juan, A. (2014). CADASIL disease: initial findings and evolution of the lesions on CT and MRI. SERAM.